The Modern Frontier of Men’s Health: Why Testosterone Replacement Therapy is Safer and More Accessible Than Ever

For decades, Testosterone Replacement Therapy (TRT) was shrouded in clinical caution and outdated misconceptions. Men seeking to reclaim their vitality, focus, and physical strength often faced a gauntlet of “black box” warnings and fears regarding heart health and prostate safety.
However, the medical landscape has undergone a paradigm shift. With landmark clinical trials and recent FDA regulatory updates, the narrative has changed. TRT is no longer just a “lifestyle” choice; it is a scientifically-backed medical intervention that, when managed correctly, offers a transformative path to optimal health.
1. The New Era of Safety: FDA Updates and the TRAVERSE Study
The most significant hurdle for TRT in the past decade was the FDA-mandated “black box” warning regarding potential cardiovascular risks. In a historic move following the results of the TRAVERSE Trial—the largest and most comprehensive study of its kind—the FDA has moved to remove these restrictive warnings.
Key Clinical Findings:
-
No Increased Cardiovascular Risk: The TRAVERSE study, which monitored over 5,000 men, concluded that TRT is non-inferior to placebo regarding major adverse cardiac events (MACE). Men on TRT did not see an increase in heart attacks or strokes compared to those not on the therapy.
-
Prostate Health: Long-standing fears that TRT “fuels” prostate cancer have been debunked by the Saturation Theory. Research now shows that once testosterone receptors in the prostate are saturated (which happens at very low levels), supplemental testosterone does not stimulate further growth or increase the risk of developing cancer.
-
Safety in Supervision: The FDA’s recent label updates (2025) reflect a growing consensus: for men with clinical hypogonadism, the benefits of normalized testosterone levels far outweigh the theoretical risks.
2. The Benefits: More Than Just Muscle
TRT is a systemic upgrade. When a patient moves from a hypogonadal (Low T) state to optimized levels, the “Positive Reinforcement Loop” begins:
-
Metabolic Health: Improved insulin sensitivity and a significant reduction in visceral body fat.
-
Cognitive Clarity: Elimination of “brain fog,” improved memory, and a more stable, positive mood.
-
Physical Performance: Enhanced protein synthesis leading to better recovery and muscle retention.
-
Cardiovascular Support: Emerging data suggests that maintaining healthy T levels actually supports vascular health and bone density, protecting men as they age.
3. Protocol Matters: The Case for Twice-Weekly Injections
One of the most common reasons men experience side effects on TRT is poor protocol design. Many local physicians still prescribe large “bolus” injections once every two weeks. This creates a “rollercoaster” effect—massive spikes in hormones followed by a “crash.”
Superior Genetix and leading TRT specialists advocate for a twice-weekly injection frequency.
-
Stable Blood Serum Levels: By splitting the dose, you minimize the “peak and trough” effect.
-
Reduced Side Effects: Frequent dosing significantly lowers the risk of estrogen spikes (aromatization) and prevents the thick blood (elevated hematocrit) often associated with large, infrequent doses.
-
Consistency is Key: “On again-off again” use is the primary cause of mood swings and hormonal instability. True optimization requires a steady, committed protocol.
4. Understanding the Risks: Misuse vs. Clinical Care
It is important to note that TRT, like any medical treatment, carries potential risks. However, the medical literature is clear: serious complications are almost exclusively linked to unprescribed use, abuse, or excessive dosing. When men “self-medicate” with black-market substances, they lack the necessary blood work to monitor red blood cell count, liver enzymes, and lipid profiles. Under the guidance of a specialized clinic, these markers are monitored religiously, ensuring the therapy remains within the “physiological goldilocks zone”—where benefits are maximized and risks are virtually eliminated.
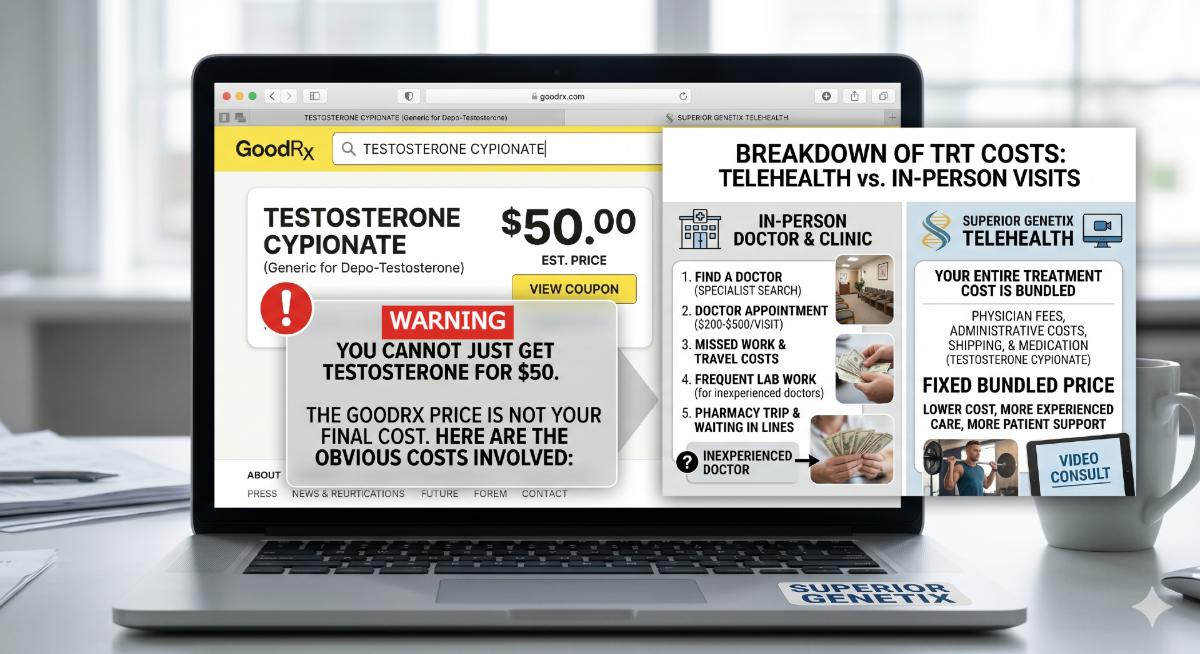
5. Telehealth vs. The Local Doctor: A Revolution in Access
Many men start their journey at a local GP’s office, only to be met with high costs and a lack of specialized knowledge.
| Feature | Local Doctor, Urologist, or Endo | Telehealth (Superior Genetix) |
| Cost per Visit | $300 – $500 (plus labs, ) | Bundled into medication cost |
| Expertise | Limited (low TRT patient volume) | Specialists (thousands of patients) |
| Convenience | Appointment weeks away
Waiting rooms |
No appointments needed
Email anytime; prompt response |
| Pricing | Expensive: frequent, unnecessary in-person visits, frequent blood work, medication cost is separate, prescriber/staff fees for every refill. No free email support. | 1 Fixed Cost: $250 includes Medication, follow-up care, prescriber fees, administrative costs, refills, monitoring, support – all included. |
| Onboarding | Very inconvenient
Manual paperwork, waiting rooms, & travel |
Easy & Hassle Free
100% Online Intake & Follow-up care |
Why Superior Genetix?
While platforms like GoodRx may show “Testosterone Cypionate” for $50, they fail to account for the hidden costs: physician consultation fees, prescribing fees, administrative overhead, shipping, and the lack of a specialized protocol.

Superior Genetix simplifies the process. They fix all physician fees, administrative costs, and shipping into one transparent price. You aren’t just buying a vial; you are buying a managed health outcome. From arranging your blood work to providing unlimited staff support, the process is designed to be frictionless.
Conclusion: Take Control of Your Vitality
The data is in: TRT is a safe, effective, and scientifically-validated tool for the modern man. By utilizing the expertise of a telehealth clinic like Superior Genetix, you bypass the high costs and outdated protocols of traditional medicine.
With all onboarding paperwork completed from your phone, and a medical team that is always an email away, there has never been a better time to optimize your hormones and reclaim your life.
What’s Included With TRT Treatment:
Physician prescribed treatment plan,Medication: Customized dosing protocol, your prescription, precisely tailored by your licensed provider, Aromatase inhibitor if medically necessary, Convenient Delivery Kit: A complete Injection Kit (syringes, needles, alcohol pads) shipped discreetly with your medication, ensuring you have everything you need to start. Hassle-Free Prescribing: Digital submission of your prescription to one of our specialized telehealth pharmacies for direct, reliable home delivery. Shipping and Handling, and easy FedEx tracking, Ongoing Medical Oversight: Blood Work Reviews: Professional analysis of necessary lab work to safely monitor your progress, Lab Work Follow-up Reports: Detailed reports, recommendations, and guidance based on your lab results, ensuring continuous, personalized adjustments to your care plan, Customized Care: Dose adjustments, implementation of other medications, Concierge Patient Support: Unlimited Email Support directly from our care team to answer questions, address concerns, and guide you throughout your entire treatment journey.
Our TRT Program Pricing Is Simply Unbeatable – GUARANTEED !
![]()
Show us a lower price and we’ll beat it.
“We Are The Lowest Priced TRT Clinic in America, Guaranteed.”
America’s Lowest-Priced TRT, Available in All 50 States
Superior Genetix the lowest-priced Testosterone Replacement Therapy (TRT) clinic in the United States. Our mission is to make life-changing treatment accessible to everyone.
Core TRT Treatment Package
Price: Just $250
This provides you with a 10 to 20 weeks of treatment—unbeatable value backed by physician oversight and support.
What Your $250 Package Includes:
- Testosterone Cypionate (200mg/mL): A full supply (typically a 10 mL vial or its equivalent).
- Aromatase Inhibitor Blend: Prescribed if medically necessary, and as part of your permanent treatment plan.
- Full Injection Kit: Syringes, needles, and alcohol pads are all included.
- Unlimited Email Support: Direct access to our expert support team for questions throughout your treatment.
- Blood Work Reviews: Comprehensive analysis of your lab results and follow-up reports via email, as needed.
Important Cost & Shipping Details (Full Transparency)
- Digital Prescription Processing, FedeEx Shipping, Handling, Tracking# — all included.
What Is Not Included (Required & Optional Costs)
- Blood Work: Labs are required twice yearly to ensure your health and safety. The cost is not included in the treatment price and typically ranges from $100–$150 per test. We partner with LabCorp and Quest Diagnostics for nationwide convenience.
- Additional Physician Consultations: $150 per appointment for any additional consultations you request outside of your required follow-ups.
- Paperwork for Private Insurance: Your prescribing physician will complete medical necessity forms for private insurance for a fee of $150.
- TRT Add-on Treatments: HCG, Gonadorelin, and Enclomiphene are an additional Anastrozole tablets are available to you at an additional cost.
How to Get Started (Simple 4-Step Process)
- Complete The New Patient Intake Form.
- Get Your Labs (if applicable).
- Pre-Appointment Consultation: Speak with one of our specialists. This is where we answer all of your questions and provide treatment instructions.
- Prescribing Physician Appointment Have a brief appointment with the prescribing physician, then pay for the treatments you select.

